How to engage your core is probably one of the most misunderstood muscle actions. Here’s an ‘Engaging Your Core 101″ for you… I hope it helps!
1. ‘Sucking in your stomach’ is not engaging your core
It’s merely shifting pressure and mass upwards or downwards. If you suck it all in hard and your waist goes narrower (it will for as long as you hold your breath anyway), all the stuff that was hanging out has gone somewhere. Upwards, pushing into your diaphragm, or downwards, pushing onto your pelvic floor. Imagine a tube of toothpaste. If you squeeze in the middle… the contents of the middle of the tube haven’t disappeared, they have moved.
Sucking in your breath or holding your breath whilst pulling your stomach in hard, is not training muscles or how to engage your core. It’s shifting pressure and displacing mass.

2. So, how do you engage your core?
You exhale, GENTLY drawing your belly button back at the same time as gently drawing your pelvic floor upwards. Your abs are drawing gently inwards, but not pulling in hard. Both the transverse abdominis and the pelvic floor are part of your core, and they work together. Making an ‘Ssssss’ sound as you exhale may help you find the right deep abdominal muscles. For the pelvic floor part… imagine you’re sucking a smoothie with your vagina as the straw… or picking up a grape with your vagina… weird. But it works.
Inhale as you relax the muscles, engage again on the next exhale. So you’re working the muscles on the exhale, relaxing on the inhale.
If you watch yourself from the side in a mirror, this shows as a very slight movement of the lower abs, not a big one. The spine is neutral, your chest should not thrust – so lower ribs stay back, stacked directly over ASIS (the hip bone bits that stick out at the front), stacked over the pubic bone. You don’t hold your breath. Your shoulders don’t tense, and very importantly, your tailbone or backside doesn’t tuck underneath you. When you isolate and engage your deep abdominal muscles, you won’t see significant movement in other parts of your body.
You could be lying on your back, on all fours, sitting or standing, but the same indicators apply – your spine should be in neutral alignment: lower ribs over hip bones, hip bones on the same vertical plane over the pubic bone. If your butt tucks under, if you suck it all in, hold your breath, thrust, tense or hunch anything else… that’s not isolating your deep abdominal muscles. Correct alignment is VITAL to making this work and is explained in detail in our programs.
3. How do you know if you’re doing it right?
Place your hands on your hip bones (also known as your ASIS) – the bony bits you can feel at the front of your pelvis on each side. Move your fingers slightly inwards and downwards from there, where it is soft. When you engage your deep abdominal muscles or transverse abdominis, you will feel a tensing of the broad flat muscle under the pads of your fingers. If your stomach pooches or pushes outwards, if you’re holding your breath, or anything is pushing away, then you’re working the outer abdominal muscles. The transverse abdominis isn’t doing its thing.
4. ‘I can feel something happening in my pelvic floor muscles’
GOOD! The transverse abdominis is part of your core muscle system, as are your pelvic floor muscles. When you draw the TA inwards, the pelvic floor should also lift. Remember, to work your pelvic floor muscles, it’s a deep lift up inside, not a little lateral squeeze at the front. Imagine drawing up the walls of your vagina and back passage (try them separately, and together… undercarriage acrobatics) as if you’re picking up a small grape and pulling it up inside you.

So, the deep core / transverse abdominis contraction is an exhale, gently drawing your belly button back to your spine, and gently lifting your pelvic floor. The pelvis doesn’t move—no tucking, hunching, thrusting or breath holding.
5. How to isolate and engage your core
…Is a necessary first stage of achieving a functioning core because you need to reconnect with it if you’re going to work with it. But it is only the first stage. We don’t do TA isolation exercises forever. Still, at first, we find and reconnect to retrain our bodies and minds to work naturally and function beautifully as they were meant to.
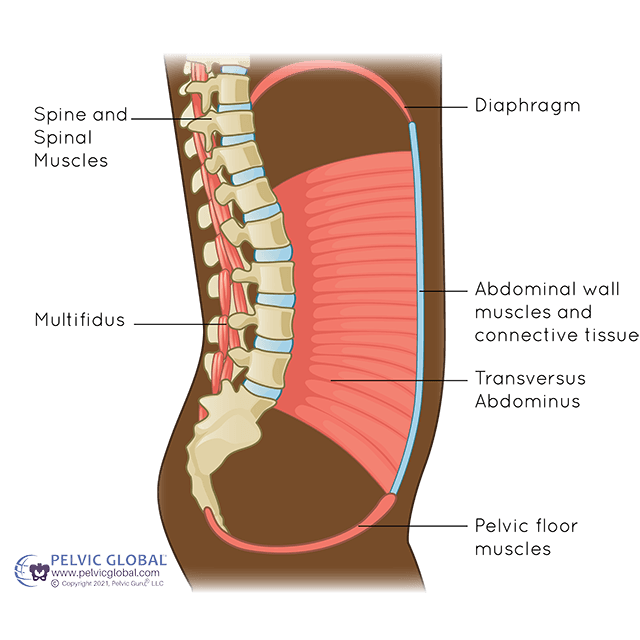
But to work, to function, the deep core is only one part (a very important part, but one part all the same) of your core system of muscles. These include your diaphragm, pelvic floor and the multifidus of your spine. Your stabilising muscles are utterly vital to your body working right. You find them, figure out how to make them work on their own, and then teach the whole system to work every time you move.
6. Intra-abdominal pressure
Intra-abdominal pressure is why your stomach muscles push out, why you get diastasis recti, hernia, prolapse and a tummy you don’t like. You need to reverse this pressure to get a tummy that looks and feels like you want it to, for the long term. This is about alignment and learning to use your entire core system right. You have to address the cause, not just the symptoms.
7. You’ve got to find it before you can strengthen it
If you haven’t found, reconnected with, and learnt to engage and use your entire core system of muscles from these foundations, no Pilates class, boot camp, binding tight things around your waist, or any other abdominal exercise is going to give you a flatter stomach.
8. Now I’ve found it, should I engage it the whole time?
No! The core muscular system’s function is to stabilise your body without you consciously contracting it every time. You need to connect, isolate, and then find and retrain it. Holding it in the whole time isn’t necessary. You don’t suck it in hard (see no.1). Hypertonic muscles are too tight – weak and tight. A constantly contracted muscle is not a strong one. So let your abs go! You ‘untuck’ and allow your pelvic floor and abdominal muscles to work through their full range of motion. This means your body finds its neutral, optimally functional alignment. To do this, the relaxing and stretching parts are just as crucial as the contracting parts.
9. If I know how to engage my core, will I get a flat stomach?
That’s because we have a layer of fat on top of the muscle. The level of body fat we carry is determined by what we eat, our hormones, emotional connections to food, and our activity levels. Stomach exercises (even the right ones) won’t give you a ‘flat tummy’. Our genetics and unique build determine our shape, as well as the curves formed by the fat and other tissue we naturally carry.
A holistic approach
This is why the MUTU System program works. It teaches you how to find the right muscles and how to reconnect with them on both an emotional and a physiological level. The latter won’t work without the former, and many of us have temporarily lost that connection. Once it all works naturally, the whole system works every time we move. MUTU teaches you how to reverse the pressure causing the problem through correct alignment. The MUTU System fills in all the gaps and missing links. It reassures and shows you why the regimes, exercises, or methods you tried before didn’t work. And why they may not have given the results you hoped for and worked so hard for.










Great article.. can you please confirm me whether I have to engage my TVA everytime I do a exercise or will it engage by itself once they get strong ?
Like if do a squat will tva get engaged automatically once they get strong ?
Hey Mayank. No. The core muscular system’s function is to stabilize your body without you consciously contracting it every time. You need to connect, to isolate, in order to find an retrain it – you do NOT have to hold it in the whole time. You definitely don’t suck it in hard. Hypertonic muscles are too tense – weak and tight.
A constantly contracted muscle is absolutely not a strong one. Let your abs go! You need to untuck your backside and allow your pelvic floor and abdominal muscles to work through their full range of movement, to help your body find it’s neutral, optimally functional alignment – and to do this the relaxing and stretching parts are every bit as important (often more important) as the contracting part.
You are not walking around permanently ‘pulled in’. You’re finding your core and re teaching it to naturally do its job. This takes patience and time, not constant sucking or pulling in. This’ll come with ongoing, consistent alignment adjustments over time, alongside the stretching and daily core mindfulness exercises that will ‘switch your core back on’.
Try to let your body move and be without tension. When you are working out, lifting or exercising, you engage on the exhale, on the exertion. But you always relax and let it go as you inhale and prepare for the next ‘work’. Don’t worry, it becomes unconscious after a while – you really won’t have to always think so hard! xx
Hi Wendy, thank you for your resources. I have a question that I haven’t been able to find the answer to anywhere. I understand that we don’t want to have our core switched on all the time so can you tell me how to maintain our posture whilst sitting at a computer or even using a standing desk? Should we engage our deep core muscles to help maintain our posture? I find that I need to but that they fatigue. A supportive chair can help to do some of the work but if standing or using a fit ball etc, there is nothing there to support the spine. I think its a problem with the activity as we are not designed to stay in the one position for a long time but that our lifestyle is requiring us to do so- driving, computers etc.
Thank your your feedback,
Libby
Hi Wendy,
I am really happy that I founf your program.I understood how to engage core muscle but I dont know how long do I have to hold the pelvis floor like do I have to keep engage through out the day?
and also is Zumba safe with your program.Instead of walking I would like to do zumba.
Hey Sapna. You can continue Zumba IF your core and pelvic floor is strong enough. i.e you don’t get any of the symptoms mention here: https://mutusystem.com/postpartum-exercise but it can’t be used as a substitute for walking. Walking is a VITAL part of the program. And finally, here’s a useful guide on engaging correctly: https://mutusystem.com/mutu-system-blog/how-to-engage-your-transverse-abdominis-muscle-correctly-flatten-your-stomach 🙂
If only it were that simple. Unfortunately, that has not been the answer to my issue, but thanks.
Can this help with urinary stress incontinence? I gave birth 13 months ago and still can’t run or do certain high impact exercises that I love. It’s really depressing.
I think kegels are the answer to your issue. They are not fun, but it works.
What about the obliques part of the question? I feel like when I’m trying to engage my TVA I’m also engaging my obliques. I guess I’m having a hard time finding my TVA… I can lift pelvic floor like a straw, draw in belly button and it slightly lifts, but it feels like the obliques are also engaged? I just finished the 12 week program and my diastasis is still a 4-5-4, has not gotten any smaller (although I am super fit now, had a personal best in a recent 5k race and actually got 3rd place for my age division, and lost weight!) About 6 weeks into the program I even started doing Sahrmann exercises in addition to MuTu to help my diastasis, I’m aware of body mechanics (keeping a flat back, not tucking tailbone under, etc.) but my diastsis persists 🙁 It also seems like simply “pulling” one’s bellybutton to spine, as many indicate, is NOT the way to engage TVA. Is there a video anywhere of how to engage tva vs. how not to that shows the difference? thanks Wendy 🙂 you are an inspiration!
Hi wendy,
I just started your 12 week program and i am so exited!
Immediately i was wondering if sex can make the diastasis larger?
I was wondering what positions are best ir worst?
Sara
Hi Wendy,
Thank you for your advice. I have a habit that I like to sit on my left side, as a result my left Transverse abdomen is bigger than the one on the right. Could you please give me any advise how to put it back again to the normal shape! if this can be possible? Thank you very much
Hi Wendy,
Thank you for your advice. I have a habit that I like to sit on my left side, as a result my left Transverse abdomen is bigger than the one on the right. Could you please give me any advise how to put it back again to the normal shape! if this can be possible? Thank you very much
You need to balance out your body by changing your movement (+ sitting!) habits – this has to be your starting point.
Hi Wendy,
Thank you for your advice. I have a habit that I like to sit on my left side, as a result my left Transverse abdomen is bigger than the one on the right. Could you please give me any advise how to put it back again to the normal shape! if this can be possible? Thank you very much
Just checking you’re in + getting answers Nicole?
Hi Wendy,
Thank you for creating a programme for us. Lying on my bed, i tried to engage the TVA and after that i got a crump in my foot (toe). Totally unrelated or not?
Also, what happens if instead of engaging the TVA im engaging the oblique (without noticing, obviiiii)? Can the diastasis get bigger? Thank you again!!
Sounds like you might be being a bit forceful there! Tight (hypertonic) muscles in your trunk or your pelvic floor (or anywhere else) are not strong … tight=weak just as much as slack=weak. And forceful sucking in or contraction will only have the effect of ‘switching off’ the deeper muscles. We isolate these muscles in the early stages of restoration in order simply to reconnect with them + establish a natural (reactive) function.
Practice working with your breath – fully (fully!) relaxing all your abdominal + pelvic floor muscles on the inhale, then drawing gently up on the exhale (think ‘picking up a blueberry with your vagina’ as the abs draw inwards). These movements are NOT big sucky-in movements, they are deep, gentle, mindful. You won’t see much happening! If you’re seeing a big sucking-in you’re going at it far too hard + simply increasing pressure. It is likely if you’re struggling that you’re being a little too forceful… breathe + relax into it. We’re not power lifting here 😉
Hi Wendy,
Thank you for creating a programme for us. Lying on my bed, i tried to engage the TVA and after that i got a crump in my foot (toe). Totally unrelated or not?
Also, what happens if instead of engaging the TVA im engaging the oblique (without noticing, obviiiii)? Can the diastasis get bigger? Thank you again!!
Sounds like you might be being a bit forceful there! Tight (hypertonic) muscles in your trunk or your pelvic floor (or anywhere else) are not strong … tight=weak just as much as slack=weak. And forceful sucking in or contraction will only have the effect of ‘switching off’ the deeper muscles. We isolate these muscles in the early stages of restoration in order simply to reconnect with them + establish a natural (reactive) function.
Practice working with your breath – fully (fully!) relaxing all your abdominal + pelvic floor muscles on the inhale, then drawing gently up on the exhale (think ‘picking up a blueberry with your vagina’ as the abs draw inwards). These movements are NOT big sucky-in movements, they are deep, gentle, mindful. You won’t see much happening! If you’re seeing a big sucking-in you’re going at it far too hard + simply increasing pressure. It is likely if you’re struggling that you’re being a little too forceful… breathe + relax into it. We’re not power lifting here 😉
Thank you for the quick response! Will do 🙂
I sent a request to join the group over a month ago, but have not received a response :-/ Is there any way you could add me because I’d love to get some help. Thank you, Wendy.
Hey Nicole, sorry about this – something much be not matching up on our database – it’ll be a slight email difference or something – so sorry. Please email my team on [email protected] + let them know. See you in the group soon!
I sent a request to join the group over a month ago, but have not received a response :-/ Is there any way you could add me because I’d love to get some help. Thank you, Wendy.
Hi Wendy. I’m new to the program and am trying to internalize the concept of engaging my TVA muscles and pelvic floor. I’m having difficulties with knowing if I’m doing it correctly. I feel like I’m trying SO hard, but am still very unsure. When you say “engage your pelvic floor”, are referring to kiegals?
I LOVE this program already and you are so relatable and helpful. Thank you!
Thanks Nicole + welcome! Please use the closed customer group on Facebook where you will get daily help from the team! https://www.facebook.com/groups/MuTu.Mamas/
Hi Wendy. I’m new to the program and am trying to internalize the concept of engaging my TVA muscles and pelvic floor. I’m having difficulties with knowing if I’m doing it correctly. I feel like I’m trying SO hard, but am still very unsure. When you say “engage your pelvic floor”, are referring to kiegals?
I LOVE this program already and you are so relatable and helpful. Thank you!
Thanks Nicole + welcome! Please use the closed customer group on Facebook where you will get daily help from the team! https://www.facebook.com/groups/MuTu.Mamas/
I sent a request to join the group over a month ago, but have not received a response :-/ Is there any way you could add me because I’d love to get some help. Thank you, Wendy.
Hey Nicole, sorry about this – something much be not matching up on our database – it’ll be a slight email difference or something – so sorry. Please email my team on [email protected] + let them know. See you in the group soon!
Thank you for the quick response! Will do 🙂
Just checking you’re in + getting answers Nicole?
Wendy, thank you so much for this excellent comprehensive guide! I am a mom of an 8yr old and 2 yr old….will be turning 44 this year….that being said, I’ve come a long way in reshaping my body….and i am currently doing a workout regimen but have terrible pelvic floor control…..everytime I sneeze or cough or do too many jumping jacks! Embarassing and highly unpleasent and uncomfortable to say the least……I fear I may not be working the right muscles as per you guide……I have lessened my mummy tummy considerably but there is still a lingering pouch….not sure what to do next….to discontinue my workout regimen, start something different? I would give anything to attend one of the live sessions but I reside in Toronto, Canada and the travelling costs and time plus the cost of the workshop would not be attainable for me at the moment…..Any guidance would be so greatly appreciated….regardless, THANK YOU SO MUCH for posting this info…sooooooo helpful!!!!
The 12 week program is what you need Paula – all is explained… 🙂 Pity you can’t come to the Masterclasses , but I’m there on video for you in the program! And thank you for your comments, you’re welcome!
Wendy, thank you so much for this excellent comprehensive guide! I am a mom of an 8yr old and 2 yr old….will be turning 44 this year….that being said, I’ve come a long way in reshaping my body….and i am currently doing a workout regimen but have terrible pelvic floor control…..everytime I sneeze or cough or do too many jumping jacks! Embarassing and highly unpleasent and uncomfortable to say the least……I fear I may not be working the right muscles as per you guide……I have lessened my mummy tummy considerably but there is still a lingering pouch….not sure what to do next….to discontinue my workout regimen, start something different? I would give anything to attend one of the live sessions but I reside in Toronto, Canada and the travelling costs and time plus the cost of the workshop would not be attainable for me at the moment…..Any guidance would be so greatly appreciated….regardless, THANK YOU SO MUCH for posting this info…sooooooo helpful!!!!
The 12 week program is what you need Paula – all is explained… 🙂 Pity you can’t come to the Masterclasses , but I’m there on video for you in the program! And thank you for your comments, you’re welcome!
Hi Wendy, I am a very visual learner at times and need to “see”. Do you have a graphic of someone standing with a tucked tailbone. I am not sure what this looks like and what I am thinking may be an extreme. Thank you!
Look down. Your ASIS (‘hip bones’ – the 2 bony markers that stick out at the front of your hips) should be directly above (in the same vertical plane as) your pubic bone. If your pubic bone is further out in front, you’re tucking. Also if your glutes are on permanent low clench (which many womens are!) you’re tucking.
Hi Wendy, I am a very visual learner at times and need to “see”. Do you have a graphic of someone standing with a tucked tailbone. I am not sure what this looks like and what I am thinking may be an extreme. Thank you!
Look down. Your ASIS (‘hip bones’ – the 2 bony markers that stick out at the front of your hips) should be directly above (in the same vertical plane as) your pubic bone. If your pubic bone is further out in front, you’re tucking. Also if your glutes are on permanent low clench (which many womens are!) you’re tucking.
Wow, I’ve been trying to get this right for a while. Read and watche videos. No one had broken it down so well. After reading this, I finally felt like I was don’t it right!
Wow, I’ve been trying to get this right for a while. Read and watche videos. No one had broken it down so well. After reading this, I finally felt like I was don’t it right!
Wow, I’ve been trying to get this right for a while. Read and watche videos. No one had broken it down so well. After reading this, I finally felt like I was don’t it right!
Hi Wendy. Can u please help me . I have a vertical gap -10 cmI think and horizontal -2 fingers. Is it very bad or is it quite normal?I started doing 12 week program, I’m on week one. Will this help me??
Hi Wendy. Can u please help me . I have a vertical gap -10 cm I think and horizontal -2 fingers. Is it very bad or is it quite normal?I started doing 12 week program, I’m on week one. Will this help me??
Ps can I do core phases 4 times per day instead of twice? Will i get more benefits if did it more than just twice or it dosen’t matter ?thank U in advance!
Beata
Hi Beata, I think I answered this below – do please use the Facebook customer group or contact the team as explained in your post-purchase emails for faster follow up that I can provide here!
Do it as often as you like – but its quality not quantity!
Hi Wendy. Can u please help me . I have a vertical gap -10 cmI think and horizontal -2 fingers. Is it very bad or is it quite normal?I started doing 12 week program, I’m on week one. Will this help me??
Hi Beata, I think I answered this below – do please use the Facebook customer group or contact the team as explained in your post-purchase emails for faster follow up that I can provide here!
Do it as often as you like – but its quality not quantity!
Hi Wendy I’m so down because I have horizontal gap _2 fingers and vertical about 10 cm. Is it very bad?? I started doing mutu system 12 weeks, im on week one. Will that help me???
Just follow the program + make sure you watch + revisit all the science workshop videos so you really ‘get it’. You can always make improvements with consistent adjustments!
Hi Wendy I’m so down because I have horizontal gap _2 fingers and vertical about 10 cm. Is it very bad?? I started doing mutu system 12 weeks, im on week one. Will that help me???
Just follow the program + make sure you watch + revisit all the science workshop videos so you really ‘get it’. You can always make improvements with consistent adjustments!
Is there a Mutu system specialist in Singapore? I have closed my gap from 4 to 1 finger 3 months postpartum but i just could not close it completely. Am eager to resume swimming with breast stroke…please help? Thank you…
Hi Ed, sorry we don’t have MuTu specialists, just our programs + live events. I would suggest you go with the 12 Week Online program
Is there a Mutu system specialist in Singapore? I have closed my gap from 4 to 1 finger 3 months postpartum but i just could not close it completely. Am eager to resume swimming with breast stroke…please help? Thank you…
Hi Ed, sorry we don’t have MuTu specialists, just our programs + live events. I would suggest you go with the 12 Week Online program
I love your idea of holistic approach . My idea is that if I am going to jump in the pool, then it should be beneficial for everything at the same time (not just today is the core, tomorrow is the back, and next week the posture). My personal experience has led me to conclude for a flat stomach I need to take the 3 layers of it into consideration : 1- the guts (eat right food, right amount, at right time), 2 – the muscles/posture 3- the fat (= working out). ..and I am in the middle of the journey to find the right formula that works for me. That being said, I’d love to learn more about your program and will look into it further.
Thanks Lababla, thats all correct. Alignment is such an incredibly important part of the process that is so often missed. You can read more here https://mutusystem.com/whats-alignment-got-to-do-with-diastasis-recti.html
I love your idea of holistic approach . My idea is that if I am going to jump in the pool, then it should be beneficial for everything at the same time (not just today is the core, tomorrow is the back, and next week the posture). My personal experience has led me to conclude for a flat stomach I need to take the 3 layers of it into consideration : 1- the guts (eat right food, right amount, at right time), 2 – the muscles/posture 3- the fat (= working out). ..and I am in the middle of the journey to find the right formula that works for me. That being said, I’d love to learn more about your program and will look into it further.
Thanks Lababla, thats all correct. Alignment is such an incredibly important part of the process that is so often missed. You can read more here https://mutusystem.com/whats-alignment-got-to-do-with-diastasis-recti.html
Hi Wendy thank you for your prompt answer. Just one more thing is it possible to see you in person or you just do this online. I live in NW London UK. My problem is I am not sure if I am doing this core engaging correctly and if the diastasis to big to be only fixed by this program. Doctors are not usually helpful with this and I was referred to surgeon regarding my umbilical hernia on 17th of July. I am not sure I want to do surgery,also I would like to try exercises first to fix the diastasis. I agree with your holistic approach and long time investment and I believe this is a route for me. The only problem is whether I will be able to understand from your instructions how to engage my core and what if I do not do it properly (that is why I asked to see you in person or if you recommend anybody in my area just for one to one one time session so I know I am doing it correct.)
Hi Tanja, I would suggest you get in touch with Camilla or one of the other London specialists listed on this page for one on one help.http://https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Hi Wendy thank you for your prompt answer. Just one more thing is it possible to see you in person or you just do this online. I live in NW London UK. My problem is I am not sure if I am doing this core engaging correctly and if the diastasis to big to be only fixed by this program. Doctors are not usually helpful with this and I was referred to surgeon regarding my umbilical hernia on 17th of July. I am not sure I want to do surgery,also I would like to try exercises first to fix the diastasis. I agree with your holistic approach and long time investment and I believe this is a route for me. The only problem is whether I will be able to understand from your instructions how to engage my core and what if I do not do it properly (that is why I asked to see you in person or if you recommend anybody in my area just for one to one one time session so I know I am doing it correct.)
Hi Tanja, I would suggest you get in touch with Camilla or one of the other London specialists listed on this page for one on one help.https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Dear Wendy,
Could you please let me know how does your system differs from Tupler technique when it comes to engaging the core and diastasis recti? Many thanx Tanja
Please see this post Tanja https://mutusystem.com/mutu-system-tupler-technique-how-do-they-differ.html
Dear Wendy,
Could you please let me know how does your system differs from Tupler technique when it comes to engaging the core and diastasis recti? Many thanx Tanja
Please see this post Tanja https://mutusystem.com/mutu-system-tupler-technique-how-do-they-differ.html
Hi Wendy, when I draw my belly button in to my spine and work on the pelvic floor, it hurts my lower back. It’s the strangest thing. Why might this be happening?
Hi Wendy, when I draw my belly button in to my spine and work on the pelvic floor, it hurts my lower back. It’s the strangest thing. Why might this be happening?
If you experience any pain at all please stop the exercises or movements that you;re doing causing the pain + see a Doctor. Ideally a specialist Physio / Physical Therapist. It sounds like you may be over tightening your muscles, or sucking in, but there are many possibilities… some hands on help will help https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Hi Wendy, when I draw my belly button in to my spine and work on the pelvic floor, it hurts my lower back. It’s the strangest thing. Why might this be happening?
If you experience any pain at all please stop the exercises or movements that you;re doing causing the pain + see a Doctor. Ideally a specialist Physio / Physical Therapist. It sounds like you may be over tightening your muscles, or sucking in, but there are many possibilities… some hands on help will help https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
When I’m engaging my TVAwhat am I supposed to engage first pelvic floor and than TVA. I seems to struggle to do it at the same time. Is breaking it into two steps an option?
Wendy, i have a lordotic curve and therefore actually need to tuck my pelvis under a little bit to achieve correct alignment. Since i also have kyphosis it gets a bit complicated to find neutral. Nonetheless i am able to draw belly button to spine by engaging the pelvic floor and i feel the “raise” in the soft part next to my hip bones when i do it. I believe i am engaging TVA. My doubt is this: I know i am NOT sucking in when i draw belly button to spine and yet if i tuck my butt under extremely i can still do it. But I thought this was impossible? You cannot draw belly button to spine if you really tuck under, right? Then why am i not sucking in and still seeing that happen?
Wendy, i have a lordotic curve and therefore actually need to tuck my pelvis under a little bit to achieve correct alignment. Since i also have kyphosis it gets a bit complicated to find neutral. Nonetheless i am able to draw belly button to spine by engaging the pelvic floor and i feel the “raise” in the soft part next to my hip bones when i do it. I believe i am engaging TVA. My doubt is this: I know i am NOT sucking in when i draw belly button to spine and yet if i tuck my butt under extremely i can still do it. But I thought this was impossible? You cannot draw belly button to spine if you really tuck under, right? Then why am i not sucking in and still seeing that happen?
When I’m engaging my TVAwhat am I supposed to engage first pelvic floor and than TVA. I seems to struggle to do it at the same time. Is breaking it into two steps an option?
Doesn’t matter a bit my Lovely. Do it however works for you… it’ll get easy I promise. The idea is that your muscles are re-learning a natural process. It’ll come. Don’t get frustrated with your body, just work with your breath, with patience + focus.
When I’m engaging my TVAwhat am I supposed to engage first pelvic floor and than TVA. I seems to struggle to do it at the same time. Is breaking it into two steps an option?
Doesn’t matter a bit my Lovely. Do it however works for you… it’ll get easy I promise. The idea is that your muscles are re-learning a natural process. It’ll come. Don’t get frustrated with your body, just work with your breath, with patience + focus.
I am learning how to engage my core. I started on my own and am beginning to make a bad habit of also tucking my tailbone every time I engage. I have a yoga instructor who is helping me now, but any advice you may have to overcome this habit and just engage the core?
Practice! Try the side on to a mirror exercise above, so you can see what your body is doing. Most likely you’re pulling in too hard + tucking your pelvis as you do so. Try a much gentler contraction on a slow exhale through pursed lips.
I am learning how to engage my core. I started on my own and am beginning to make a bad habit of also tucking my tailbone every time I engage. I have a yoga instructor who is helping me now, but any advice you may have to overcome this habit and just engage the core?
Practice! Try the side on to a mirror exercise above, so you can see what your body is doing. Most likely you’re pulling in too hard + tucking your pelvis as you do so. Try a much gentler contraction on a slow exhale through pursed lips.
Honestly, i feel the TVA’s more so when I actually bear down rather than sucking in when I exhale.
Bearing down increases intra abdominal pressure, which is the opposite of what you want. the pelvic floor is lifting as TVA is engaged correctly, so if you’re pushing or bearing down, that not engaging TVA correctly.
Honestly, i feel the TVA’s more so when I actually bear down rather than sucking in when I exhale.
Bearing down increases intra abdominal pressure, which is the opposite of what you want. the pelvic floor is lifting as TVA is engaged correctly, so if you’re pushing or bearing down, that not engaging TVA correctly.
It is important to build muscles. Muscles signify a fit body. Achieving
that sculpted body means knowing the right kind of muscle building
workouts.
The first step in the workout is to perform strength exercises. This can
either be using free weights or body weight. This is to ready the body
for more strenuous routines later. More calories are burned
It is important to build muscles. Muscles signify a fit body. Achieving
that sculpted body means knowing the right kind of muscle building
workouts.
The first step in the workout is to perform strength exercises. This can
either be using free weights or body weight. This is to ready the body
for more strenuous routines later. More calories are burned
Hi, I’m a larger girl and I am really worried that I am not doing my TVA’s properly because when I do them, I do feel as though I’m sucking in, but I think that’s just because I have a lot of fat around my mid section. How can I know I’m doing them properly?
This post above explains what you should or shouldn’t be feeling Chris – for a deeper explanation I would recommend you try one of our programs. The fat on top shouldn’t really matter… the muscles are going on underneath even if you can’t see them! If you fee like you;re sucking in… you’re probably sucking in though!
Hi, I’m a larger girl and I am really worried that I am not doing my TVA’s properly because when I do them, I do feel as though I’m sucking in, but I think that’s just because I have a lot of fat around my mid section. How can I know I’m doing them properly?
This post above explains what you should or shouldn’t be feeling Chris – for a deeper explanation I would recommend you try one of our programs. The fat on top shouldn’t really matter… the muscles are going on underneath even if you can’t see them! If you fee like you;re sucking in… you’re probably sucking in though!
Thanks for the interesting article!
Glad you found it helpful 🙂
Thanks for the interesting article!
Glad you found it helpful 🙂