You may have heard the term “vaginal mesh surgery” or “pelvic mesh surgery”. It’s been discussed in the media, by health professionals and maybe even by women in your circle of family and friends. By getting informed and educated, you are empowered to make informed decisions about your own recovery.
What is vaginal mesh surgery?
Vaginal mesh surgery a.k.a. pelvic mesh, transvaginal mesh or the urogynecological mesh, has been used in the surgical treatment of Stress Incontinence and Pelvic Organ Prolapse since the late 1990s. Medical professionals use this option when other options haven’t worked.
Stress incontinence
Stress Incontinence (SUI) means you pee yourself when you exercise, sneeze, laugh or do certain activities. A little or a lot of pee, it doesn’t matter. This is Stress Incontinence. It doesn’t feel good, it can make you feel embarrassed, lonely, disconnected from your body and maybe even let down by your body. Incontinence is a common condition affecting 1 in 5 women1). Common but NOT normal. Let’s be clear, leaking of any kind, just because you had a baby or because you are a woman of a certain age, is not something you have to put up with. You deserve better.

Pelvic organ prolapse
Pelvic Prolapse, Pelvic Organ Prolapse or ‘POP’ is caused by the weakening and/or damage of the muscles, ligaments and tissues which make up the pelvic floor and hold the pelvic organs in place. It acts kinda like a hammock, supporting your bladder, uterus and bowel. Prolapse affects 50% of women who have had children(2).
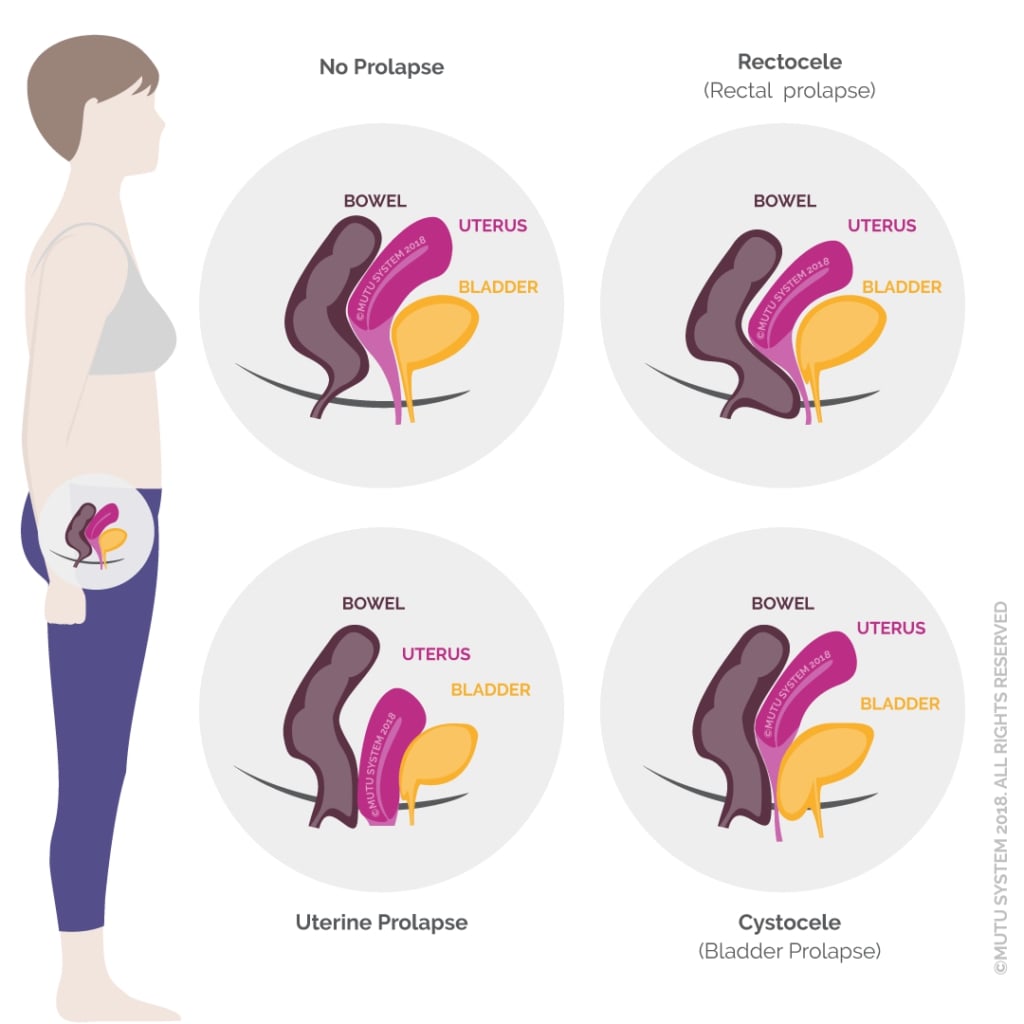
There are different types of pelvic organ prolapse:
❌ cystocele (bladder prolapse)
❌ rectocele (rectal prolapse)
❌ enterocele (small intestine prolapse)
❌ vaginal prolapse
❌ uterine (prolapse of the uterus).
Prolapse symptoms
Pelvic Prolapse symptoms can leave you feeling pretty sucky mentally and physically, Symptoms include pressure or pain in the vagina, rectum, or both. Feeling like your “insides are falling out”, urinary or faecal incontinence, constipation, back pain, abdominal pain, lack of sexual sensation, painful sex, and not being able to keep a tampon in.
The vaginal mesh surgery controversy
Recently, there’s been a lot of controversy surrounding vaginal mesh surgery. While the mesh has been an effective form of treatment for some women, there are also many women who have experienced extremely serious and sometimes life-changing complications, including:
❌ mesh erosion
❌ the mesh cut through the internal tissue resulting in vaginal scarring
❌ fistula formation
❌ painful sex
❌ pelvic, back and leg pain.
Often these complications occurred years after the surgery and have become difficult to treat.
The mesh went through clinical trials before its introduction, which showed a low level of complications, but this data has now come into question.
Out of over 2,220 women who had undergone vaginal mesh surgery or pelvic mesh repair, 59% said the procedure had not resolved their initial symptoms and 58% said they were left experiencing pain during intercourse (3).
Law suits, long term damage and trauma
The creators of this mesh are now facing many lawsuits. Our heartfelt sympathy, support and love go out to all the women who were let down and had to suffer the devastating consequences of this regulatory failure.
Every woman deserves the dignity of a body that works and that makes her feel good. We believe in giving you the right information and education so that you can make your own informed decisions about your body and your recovery.
At MUTU our goal is to empower women using natural, proven and holistic techniques.
So that you can take control of your recovery, gain knowledge and information to strengthen your pelvic floor in the comfort of your own home.








