Pelvic Organ Prolapse (POP) doesn’t only happen to older women, it happens more than you might think.
❗️50% of women of childbearing age will experience some level of Pelvic Organ Prolapse❗️
What is Pelvic Organ Prolapse?
TL;DR? Any kind of prolapse means that one or more organs of your abdomen or pelvis have dropped or shifted position. This can result in discomfort or lack of healthy function.
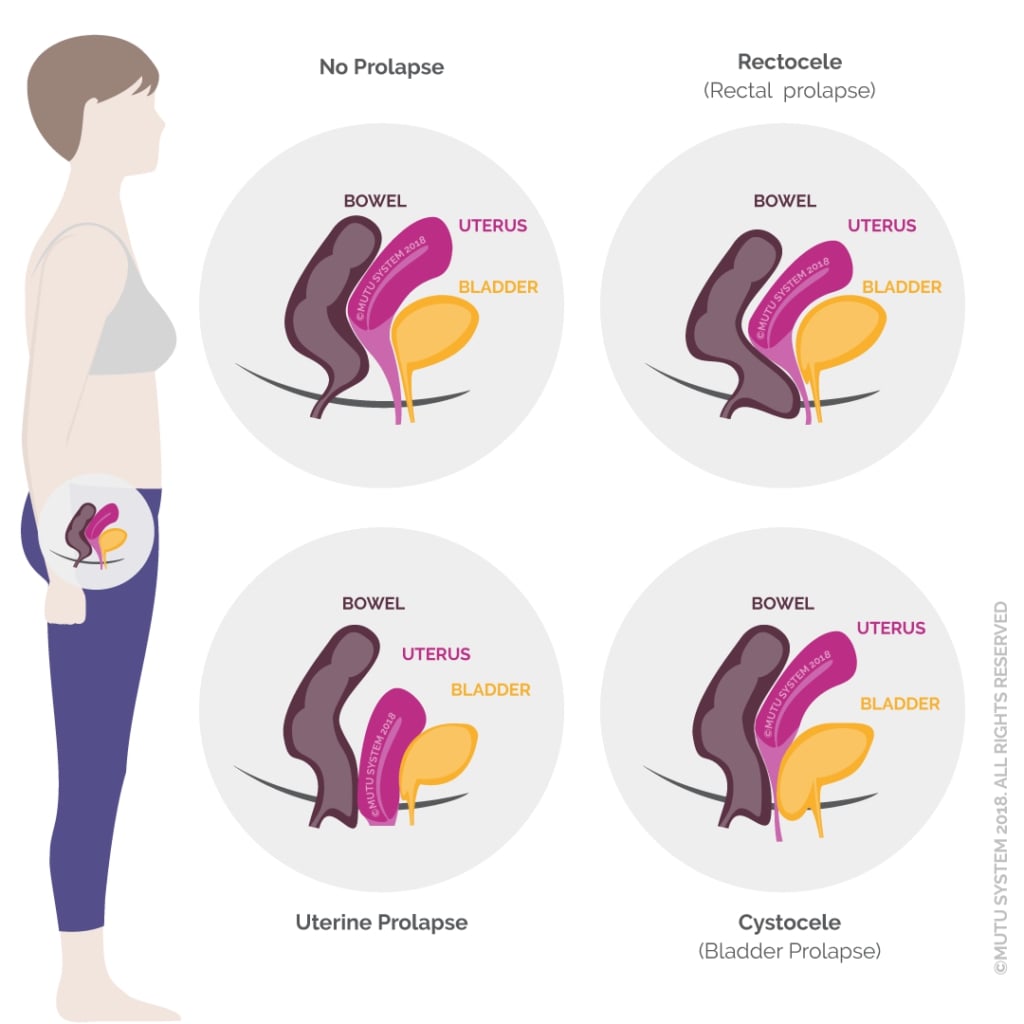
There are 5 types of pelvic organ prolapse: cystyocele (bladder drops and bulges into the vaginal canal), rectocele (large bowel or rectum bulges into the vaginal wall), enterocele (intestines), vaginal vault (vagina caves in on itself, possibly after uterus is removed-hysterectomy), and uterine (uterus drops).
It is measured in Grades 0-4. 0 is normal or optimal positioning, 1 or 2 may result in mild or moderate symptoms but are unlikely to require surgical intervention, Grade 4 refers to a prolapse that has actually protruded right outside of the body.
Prolapse Symptoms
How do you know if you have it? Each of these 5 types of prolapse has its own symptoms, but in general, symptoms can include:
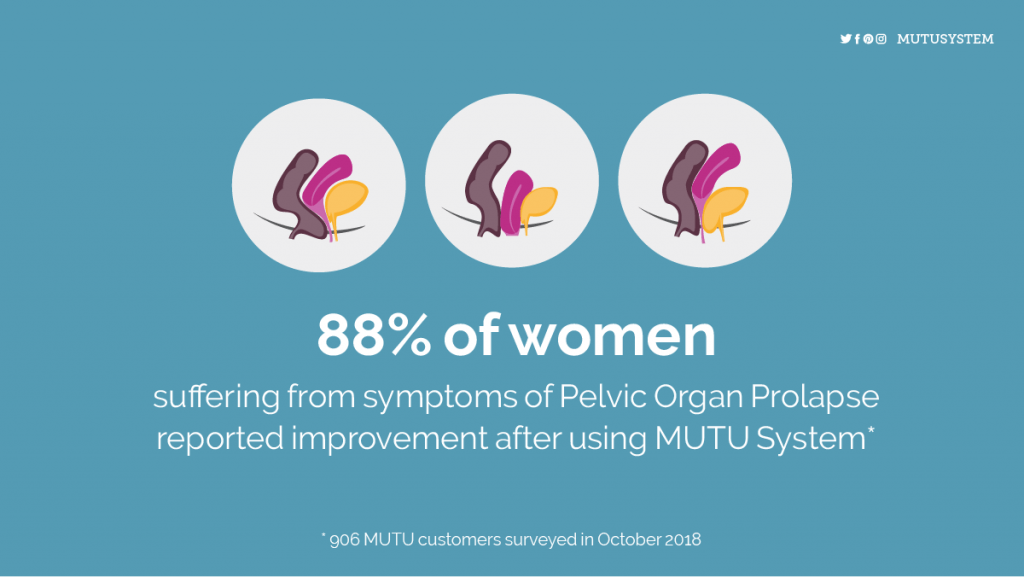
- Pressure, pain, bulging or fullness in vagina, rectum, or both.
- Feeling like your “insides are falling out” or like you are sitting on a ball.
- Urinary incontinence.
- Urine retention (you have to pee, you just can’t get it to come out).
- Fecal incontinence.
- Constipation.
- Back/abdominal pain.
- Lack of sexual sensation.
- Painful intercourse.
- Can’t keep a tampon in.
It feels pretty horrible and it may be something you don’t feel comfortable talking about, so… Here’s everything you need to know.
What causes pelvic organ prolapse?
Prolapse, Hernia and Diastasis Recti are related conditions in that they are all caused by excessive pressure inside your abdomen and pelvis. The pressure pushes everything away, outwards and downwards.
It’s the job of your core and pelvic floor muscle system to keep this natural pressure contained so that your abdomen and pelvis can function how you want them to. But if alignment or posture has shifted, if you had a prolonged or complicated birth, or if you’re just getting older, the pressure might be ‘off’.

Pregnancy doesn’t cause prolapse and neither does simply a weak pelvic floor. However, there is no question that prolonged labor and pushing, or medical intervention such as forceps or ventouse, may increase the likelihood of prolapse occurring.
What can you do to prevent or relieve symptoms?

Important! A prolapse will not inevitably worsen, so if you are suffering from Grade 1 or 2 symptoms, preventative and healing strategies and changes can prevent your prolapse from escalating.
The solution involves, but is not isolated to, your pelvic floor. Here are some ways you can start to correct the pressure inside your abdomen and pelvis right away and start to reverse the symptoms AND CAUSES of pelvic organ prolapse:
Alignment and pelvic organ prolapse
Alignment means your bio-mechanics, your posture, or how to sit, stand, and move.
Try not to tuck your backside underneath you, or walk in high-heeled shoes all the time, which thrusts your pelvis out in front and strains your hip flexors and knees. Notice if you bend your knees all the time when you stand or stick your chest out or your chin up. We work a lot with your alignment in MUTU, as it’s truly the foundation of a healthy core and pelvic floor. Read more about alignment and your pelvic floor here.
Think of a hose pipe that gets a kink in it. The water inside is now placed under increased pressure as free flow is prevented. It tries to find ways to escape. Pressure builds up and seeks the weakest point. This is what happens in your body when we move in a ‘kinked’ alignment, and diastasis, hernia, or prolapse may result.
Engage your core correctly
The full deep dive on How to Engage your Core Correctly here.
Change the way you go to the toilet!
The Western toilet does not offer a good position for elimination – whilst a full squat is much more functional and comfortable.
We frequently and proudly recommend the Squatty Potty – (mostly for the unicorn 🌈 🦄…and the handsome prince 👑LOL). Recreate a more natural posture by raising your feet to angle your pelvis and pelvic organs to eliminate easily, completely, and without strain. It’ll change your life…. Like, actually.
What about squatting – isn’t that bad for prolapse?
We squat a lot in MUTU – it’s a functional, natural, load-bearing (bone strengthening) and glute-building core exercise. What’s not to love? For a healthy and strong pelvic floor need to prevent prolapse, our glutes need to be strong and sacrum needs to be flexible and hanging in space, not all tucked under you so your pelvic floor muscles are shortened.

To squat correctly, your shins should be vertical, but not tucked underneath, weight through your heels and the outsides of your feet.
Squatting precautions: If you feel bearing down or discomfort in this or any other exercise, STOP and consult with a specialist. MUTU is recommended for prolapse by specialist Physical Therapists. MUTU has video instructions of modifications for all exercises. If you feel any heaviness or discomfort, get advice for your individual circumstances, and don’t squat deeply.
Kegels (how to get them right)
To re-connect and identify the right muscles, you need to isolate and focus on them. On an exhale, try that little squeeze at the front where you wee, then on the next exhale lift the middle – your vagina, then on the next, lift your back passage, imagine drawing your rectum up inside. Don’t clench your butt (this is hard!).
Try these pelvic floor acrobatics a few times to focus on the 3 openings of your pelvic floor and re-connect your brain’s nerve pathways to the muscles. Go front, middle, back… then back again!
Whilst Kegels or traditional pelvic floor squeezes may ‘tighten up’ your pelvic floor muscles in the short term they are simply not enough, and there is a vital element missing in the way these are often performed. The relax phase of any muscle action is every bit as important as the contract phase, and nowhere is this more pertinent than in the case of your pelvic floor. A hypertonic (too tight) pelvic floor is equally as likely to be the problem as a ‘too loose’ pelvic floor. So if when you are Kegel-ing you are doing any of the following: bending your knees, tucking your backside under, or clenching your butt muscles… you’re not actually getting to the deep pelvic floor muscles at all.
Why kegels aren’t enough: The science bit
TL;DR? You need a strong and healthy pelvic floor to help keep your organs inside your body and functioning normally. You need a strong and healthy pelvic floor to prevent leaks and discomfort. But think of your perineum as the ‘trapdoor’. You also need strategies to keep your organs suspended, ‘hoisted up’ where they’re supposed to be. Thats about alignment and pressure. Just squeezing your pelvic floor won’t cut it.
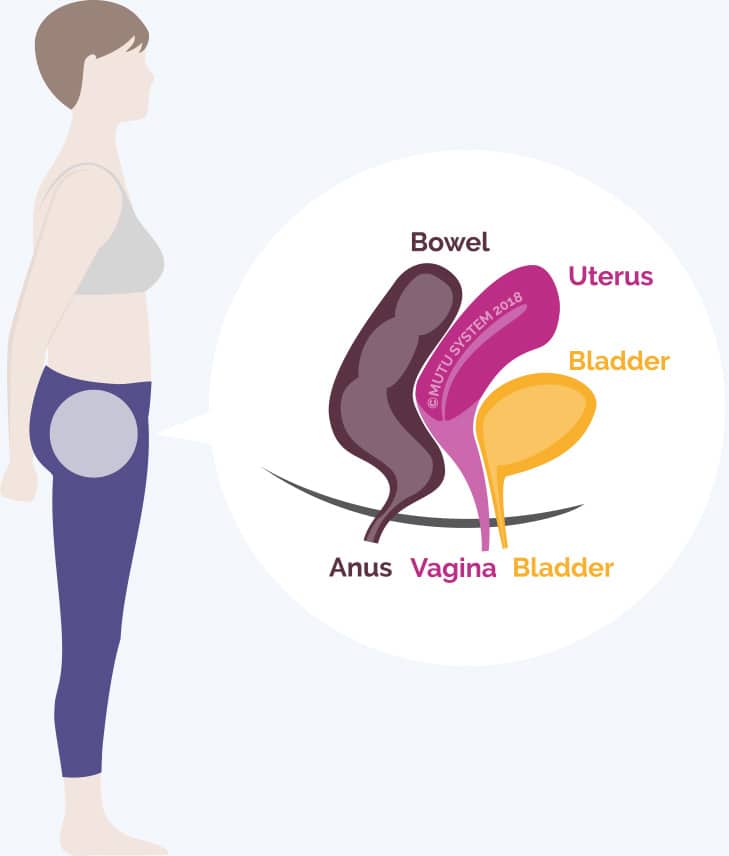
You see it is not only your pelvic floor muscles’ job to ‘hold everything up’ – You have a complex system of fascia and ligaments that hold your organs suspended in their optimal positions inside your pelvis. Think of them as the puppeteer’s strings.
This applies to all the pelvic organs that have their openings at your pelvic floor – your vagina, uterus, bladder and rectum… none of these organs are reliant solely on your pelvic floor to do all the holding work, so, therefore, to focus only on squeezing your undercarriage like crazy can only ever be a band-aid or a temporary distraction from a much more serious problem: that your pelvis is not containing your organs effectively and they are heading south. Pelvic floor exercises are important, but they’re not the whole story.
Of course, your pelvic floor muscles are fundamental to the whole ‘Prolapse’ conversation. They’re integral, forming the undercarriage of the cavity which houses all these organs.
The whole core muscle system is involved
At the top of that cavity is your diaphragm muscle, and the deepest muscle that wraps around the sides is your Transversus Abdominis muscle. At the back are the Multifidus muscles of your spine. Your Transversus Abodminis muscles sit beneath your obliques and run across the sides of your waist. In the middle of your abdomen, you have the Rectus Abodminis muscles also known as the six-pack muscles.
When the intra-abdominal pressure builds or is not contained effectively by the core muscles, due to excessive straining or pushing, poor alignment, aging or a combination of factors, it gets too much. Whilst our bodies won’t actually explode… something still has to give. It might be a hernia popping out at the weakest point, it might be a widening of diastasis recti, or the force may go downwards, pushing and shifting pelvic organs downwards and in severe cases, actually out of our bodies.
That’s Prolapse. When your supportive core muscle, fascia, and ligament structures can no longer hold one or more of these organs in place, they descend. Whilst a ‘weak pelvic floor’ didn’t exactly help the situation, it didn’t single-handedly cause it either.

Further resources for pelvic organ prolapse support
If you suspect you have a prolapse, we recommend you seek one-on-one specialist help from a Women’s Health Physiotherapist / pelvic health PT.
Pelvic Organ Prolapse Support (APOPS)
From Tracy Sher at the Pelvic Guru, The Ultimate Pelvic Anatomy Resource! Links, articles, and videos – this post is kept updated – an amazing resource.
Downloadable (free) PDF information leaflets and diagrams available from the International Urogynecological Association (IUGA) (click ‘Patient Leaflets’)
The Pelvic Partnership | Great resource for pelvic pain in pregnancy.







Hi. What can I do to reverse or get my pelvic organs back into place? I was told the POP is grade 2. Really upset with this news. Thanks!
Hi Cathy, Thanks for your message.
We are absolutely not medically trained nor qualified in any way to diagnose, assess or even give an opinion on your personal condition. We cannot comment on your individual medical circumstances by personal email. We encourage you to please do the following, in order of urgency:
If you are in ANY pain during or after exercise, please cease the activity immediately and do not return to it until you have consulted with a medical Doctor. Put simply, if something hurts, stop doing it and don’t do it again until you have discussed your program and agreed a course of action with your Doctor.
If you have unexplained discomfort or lack of function anywhere in your abdomen or pelvis, we strongly recommend you consult with a Women’s Health Physiotherapist or Pelvic Physical Therapist for individual assessment, diagnosis & movement prescription.
This page gives you detailed information on how to know when you may need specialist help, and how to find it. If you are suffering with SPD, PGP, hernia or prolapse, or if your diastasis or connective tissue is not responding to the consistent practice of the MUTU restorative work, then an individual assessment by a medically trained, specialist Physical Therapist is recommended. We cannot advise beyond the scope of our programs. Please be assured that MUTU is recommended by Physical Therapists around the world and that we actively encourage you to share the program with your medical caregiver to have them help you with appropriate adaptations or omissions.
Hi Wendy,
my lil one is 6 months now, imp to mention i had a c- section so i could not do core exercise. However, with a healthy diet and breast feeding, i have lost 12 pounds.
But it does not make me fee better. My belly is pooched out and i always have an uncomfortable feeling in the abdomen. I keep wearing a PP belt but it does not make any difference, infact i can feel the sagging skin around my belly bottom. It is very very annoying. I miss my pre-pregnancy body, it was wonderful. i was fit and healthy. Please suggest me, how to get my body back ….
Hey Shova, I’m sorry you’re feeling down. But you can be fit and healthy again and feel good about your body – try to focus less on getting ‘back’ your body before you had babies, and focus instead on strengthening and nourishing the body you have now. MuTu will help you on all levels – the foundational exercises to get your strong, the nutrition you need, and moving onto more intensive (but safe) workouts… as well as the encouragement, reassurance, confidence and motivation you need x
Thank you, Wendy. I already purchased your MuTu Focus Program and just started it today. But I will take your advice and see a pelvic physical therapist as well. 🙂
I feel like I’ve been butchered after a hurendous episiotomy 10 weeks ago. I now have a prolapsed bladder that protrudes at the opening of my vagina and suffer from chronic back pain, pains in my vagina, some incontinance soreness and chafing not to mention emotionally being affected by this condition and not being able to go about daily activities without pain. I have seen my GP, then a consultant and was fitted with two ring pessaries both of which slipped out of place. Consequently, I have been informed that this is no longer a suitable option and the only other suggestion is a cube pessary.
I feel desperate and miserable. I have been told it should reverse given time, and to use a pessary and do pelvic floor exercises in the meantime. However, most research I have read states that a grade 3 prolapse is unlikely to improve with pelvic floor exercises and will need surgery. Also I have been informed that because I am breastfeeding improvement will take longer. The physio suggested to do pelvic floor exercises which I had already been doing (confident that I am doing them correctly). I have looked up the ‘cube’ which looks unpleasant and I’m beginning to feel like I shall never be normal again or have a physical relationship with my husband.
Is there anything else I could be doing/trying to make life more bearable and treat this condition? What about electrical stimulation would this help? I just want to recover and get on with the job of being a mum, which this condition is also affecting. Any suggestions greatly received.
Hey Collie,
So sorry to hear you’re feeling miserable. My suggestion for you would be to seek out a specialist women’s health physiotherapist. They’ll be able to properly diagnose and guide you through your options and recovery.
Check out my page on referral to a women’s health physio here: https://mutusystem.com/referral-to-a-womens-health-physiotherapist
Sending you lots of healing hugs xx
Hi! Five months after I gave birth I noticed a prolapse which I suspected a rectocele after doing some research. I tried doing kegels thinking it will solve the problem since I didn’t have any pain nor symptoms or difficulty. At ten months I went to see my midwife and had her checked it and she confirmed I have a grade 2 rectocele. She referred me to a pelvic floor therapist but I haven’t had the chance to make an appointment. A midwife friend recommended your program and I just finished reading about the focus program but I wanna make sure before I purchase it that it is the right program for me. Thank you!
Hey Richel,
Thanks for your comment and for stopping by on the blog! I’d absolutely recommend that you make an appointment as soon as you can to see your pelvic physical therapist. They will be able to guide you through treatment and recovery for prolapse.
No exercise program can or should claim to cure or ‘fix’ a hernia or prolapse. These conditions should be diagnosed and treated according to your medical Doctor’s recommendations.
MuTu System core and breathing exercises, progressed gradually, mindfully and over time, are gentle, restoring and healing. They are likely to be an ideal complement to your Doctor’s recommendations. Intensive or high impact workouts should be avoided completely if you have hernia or prolapse. Only MuTu Focus, or the Core exercise sections (i.e. NOT the intensive workouts) of the 12 Week Program may be beneficial with your Doctor’s approval.
You should of course seek and follow your medical caregiver’s advice regarding diagnosis and options for treatment for these conditions. Severity and necessity of medical intervention vary widely and should be discussed with your doctor.
Hernia, prolapse and diastasis recti are all results of excessive intra-abdominal pressure. This means that your abdominal and pelvic cavity cannot withstand the pressure within, resulting in pushing away, out or down at the weakest points – such as your pelvic floor or the mid-line of your abdominal muscles. By adjusting your alignment to allow your body to support itself more effectively and your muscles to work optimally, along with learning to connect with and engage the deep muscles of your core and pelvic floor… you can enable your core to become stronger and more stable.
The MuTu System Focus Program is likely to be safe for you, but should be conducted only with your health care provider’s knowledge and blessing.
If you are suffering with hernia, pelvic organ prolapse (POP) or any pelvic or abdominal discomfort or pain, MuTu System Limited expressly recommends you do not start any exercise program without individual medical diagnosis and advice.
Hi Wendy, Thank you so much for this information and for your program! I am currently pregnant with baby #2 and am on week 6 of your 12 week core program (I’m hanging out at week 6 for now). I definitely didn’t “put myself together” after baby #1 (he was big, 4240g, natural birth). I’ve noticed that in the last month of doing the program the “bulge” down under has gotten more pronounced. This also coincides with a period of rapid fetal growth and belly expansion of pregnancy (I’m 24+ weeks currently). I’m doing the core and trying to use appropriate alignment (I’m actually a PT so I am in tune with the general postural alignment, but not a women’s health PT so the pelvic floor bit takes some serious focus). I plan to see a women’s health physio post partum, but am not sure if I should go sooner, dial back on the intensive workouts, or just really focus on the pelvic floor. Since it’s all connected I will let you know that whilst my gap has closed thanks to your program (from 3 fingers to 1!), the connective tissue support in the middle has disappeared as my belly has grown (I used to be able to feel the connective tissue when testing DR and had gotten it from full finger to first knuckle depth, now it is back to full finger depth). Any thoughts? Thanks!
Hey Sarah.
Congratulations on your pregnancy!
Testing for a diastasis recti during your pregnancy is really not necessary. Whilst you can minimise the impact of diastasis on your core muscles by working on alignment and core strength during pregnancy, don’t go poking about in your bump or worrying about diastasis recti or abdominal separation during your pregnancy.
The rectus abdominus muscle parts in a third of first pregnancies, and in around two thirds of second or subsequent pregnancies. We’d rather it didn’t, but it is common, and being aware of and adjusting your alignment and the mechanics of how you carry your growing bump will help comfort now and recovery afterwards.
What you can do is work on your alignment and keep your transverse and pelvic floor muscles supple and strong throughout pregnancy, whilst avoiding exercises or movements that will exacerbate the problem. You can make changes to your alignment to reduce intra-abdominal pressure and to ensure that your whole core is carrying your growing baby, rather than all the pressure being out front and straining at the weakest point. This will ensure the effective recovery and restoration of those core muscles after the birth, and make repair of the gap easier.
Keep your body strong, aligned and working in the right direction… and most women will be able to repair the gap painlessly in 6-12 weeks. Please do all of this with the consent of your midwife or doctor. This varies from woman to woman and MuTu might not be suitable for certain women during pregnancies. Just double check.
xxx
Hi. I have questions:-). Very long story short, i have a mild cystocele and moderate rectocele. however, the specialists refused to do surgery saying it wasnt bad enough. I spent a year with a specialist physio, with nil discernible effect. I was a distance runner (marathons) and was well into weighlifting.
Now because of the discomfort of the prolapse I struggle to exercise. I have gained 30kgs in the 3 years. I have a new wave of motivation. The specialists cannot or will not help me. Pelvic floor exercises did not help, nor did specialist physio input.
Can you suggest anything that may help? I’ve signed up for a half marathon in november and im determined to do it. The only advice i got from the consultant was to make it worse so that they can fix it….
Thank you very much for all this information.
It is fantastic to know that there is more beside kegels
You’re welcome Cindy!
I know you feel embarrassed my love, but the longer you leave it and ignore a problem like this the worse it gets. My advice would be get to your doctor as soon as you can, if you feel more comfortable request a female doctor or click the link in my previous comment to see a list of professionals who deal with stuff like this on a daily basis. Sending you lots of love and encouragement. 🙂
I’m not sure I could even speak to my doctor about it. Thanks for replying though!
Hi, not sure if this is the right place for me – never had children, 23, always been overweight/obese (this can weaken those muscles?) And recently noticed I’ve been leaking wee when I laugh, cough ect, so I’ve looked into doing kegels (also noticed yesterday I can’t stop the flow of wee when trying to find the kegel muscles anymore…) I also feel there’s a bit of a difference in my vagina walls – bulge out a bit when I squat or sit on the loo or stand – I can’t feel it happening, just with my fingers I feel it. However I’m not sure if this is normal or has always done this and I’m just worrying about it. I feel v embarrassed about this & I doubt I would be able to bring it up with a doctor. I wanted to ask if the ‘squeeze & life” kegels would be right for what is wrong with me, or would all the exercises listed on here be better? I read them but find them a little hard to follow, I don’t have a exercise ball either. I also wanted to ask if I do kegels and my belly muscles ache slightly the day after, am I doing them wrong? Thank you
Hi Kay. This is something you need to speak to your doctor about and look at getting a referral to a WOmen’s Health Physic: See this link: https://mutusystem.com/referral-to-a-womens-health-physiotherapist
The MuTu System program (while designed for Mums) will still be highly beneficial for you and will help to strengthen your pelvic floor and core. It’s not normal to leak when you laugh or cough and you can do something about it. Your first port of call should be to speak with your doctor, check they are happy for you to embark on the program and ask if you need a referral. 🙂
I am a 47 yr old mother of 7 ( with all babies weighing 8lbs or more- largest was 9lbs 11 oz. )
Had total organ prolapse. Tried pelvic floor therapy , helped some but not enough. Pressure was felt after standing for anything longer than 45min. I ended up being referred to a urogynocologist who after one examination suggested surgery. I agreed and underwent robotic surgery to remove uterus, and fix my bladder and rectal prolapses. It’s been a year and so far results have been great! No more pressure and I can function throughout my day w/out constant bathroom breaks and/or leakage.I know my pelvic muscles are still very weak and I have a belly bulge that has remained since surgery.
I am interested in the Mutu program. My question is, would your program work for me? If so, which one would you recommend? Should I consult my doctor before I start?
* as a side note** I want to say Thank-You for all the info you make available. After reading some of the articles you post, I have stopped some of the exercises I was doing like leg lifts, crunches, and planks.
Hey Corina. Thanks so much for stopping by and for your message. I’m so pleased you now feel much better and yes, the program will indeed by highly beneficial and help you to strengthen the core muscles and pelvic floor. It’s something you can keep doing to maintain that strength going forward.
Yes you should absolutely consult your doctor first before you embark on any exercise program to make sure they are happy for you to exercise and that the exercises are suitable for your individual medical case. The Focus program is purely the core and pelvic floor exercises and the 12 week program includes the same core and pelvic floor exercises but also includes more intensive fat burning exercises. If you’re doctor is happy for you to do more intensive stuff eventually, I’d say go for the full 12 week program and you can progress at your own pace when you feel your body is ready.
You’re so welcome. I’m really pleased you’ve found some of my articles useful. Best wishes, Wendy.
Hi Amanda, Focus or the Core phases of the 12 week program are the safest options for you at this stage. If you do buy 12 week you can just stay on the Core phases 1 and 2 until you are given the go ahead from your physio to move on.
I am so happy I found this article…I have been going back to the doctor from some time and he said it was nothing he can do about this…i tried going to a PT…but no relieve…so i join a gym and i am doing things at home…Does it ever go away?…Is this something i have to deal with for the rest of my life…im only 31..
Danielle. No – it’s not something you have to deal with for life. Have you been referred to a women’s health Physio? Check out this page here: https://mutusystem.com/referral-to-a-womens-health-physiotherapist
You never talk about pessarys for prolapse-I have been wearing one for two years-the first year went great but now I’m one my second year and have had vaginal E Coli-yeast from the antibolic-then another unknown bacteria which needed a vaginal gel treatment for 5 days and a sore has developed inside my vagina-now I have to leave the pessary out for two weeks for healing to occur. Are pessary a good option?
Yes absolutely, as advised and on the guidance of your women health physio or pelvic PT. Pessaries are a non surgical solution that help many women. However they are always be used in conjunction with restorative pelvic floor exercises as in MuTu of course and always with expert guidance.
Hi my names teagan i have a slight bladder prolapse,my doctor reccomened the ball exercise that you insert,my vagina is pushing these balls out as it does with tampons or anything,my bladder is getting worse as i age im only 30 and constantly dribbling wee out all the time,ive had 3 kids but prior to mids i have always had a weak bladder, i want to fix it now ive just had enough help pls
Hi Tegan. Take a look at this article here: https://mutusystem.com/referral-to-a-womens-health-physiotherapist. With your doctors approval the Focus program or the core phases of there 12 week program can help to strengthen your pelvic floor and core gently and safely.
Hi my names teagan i have a slight bladder prolapse,my doctor reccomened the ball exercise that you insert,my vagina is pushing these balls out as it does with tampons or anything,my bladder is getting worse as i age im only 30 and constantly dribbling wee out all the time,ive had 3 kids but prior to mids i have always had a weak bladder, i want to fix it now ive just had enough help pls
Hello! Thanks for your expert advice!
I’m hoping you can help me with a few questions:
What do you recommend as far as repetition for the exercises and how many sets a day?
How soon could one expect to see improvement of the condition while following these exercises? Days? Weeks? Months?
Would you recommend abstaining from exercise while experiencing a prolapse? I’m currently nordic skiing, running and walking.
Thank you!
Hi Jordan,
My guidance on exercise and rep is included in the program. You spend 10 minutes twice a day on the core phases. In terms of stopping exercise you would need to discuss this with your doctor but generally if you feel uncomfortable, if you experience any leaking, if something doesn’t feel quite right, if you have POP, stepping back from intensive exercises is wise.
Hello! Thanks for your expert advice!
I’m hoping you can help me with a few questions:
What do you recommend as far as repetition for the exercises and how many sets a day?
How soon could one expect to see improvement of the condition while following these exercises? Days? Weeks? Months?
Would you recommend abstaining from exercise while experiencing a prolapse? I’m currently nordic skiing, running and walking.
Thank you!
Hi wendy
I have had a slight bowel prolapse for a long time but have been experiencing more problems recently my physiotherapist has suggested your DVDs .I am struggling to decide which one is the best .thought maybe the focus? What would you suggest.
Thank you
Amanda
Hi wendy
I have had a slight bowel prolapse for a long time but have been experiencing more problems recently my physiotherapist has suggested your DVDs .I am struggling to decide which one is the best .thought maybe the focus? What would you suggest.
Thank you
Amanda
Hi, I have been told i have first degree bladder prolapse and DR (with 4 fingers gap) and weak back — I have a 12 week old and very keen to join the program… I wonder if i am fine to join the program ?
Thanks
Please refer to this post https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html Our programs are likely to compliment your care but prolapse should be discussed with a medical professional first
Hi, I have been told i have first degree bladder prolapse and DR (with 4 fingers gap) and weak back — I have a 12 week old and very keen to join the program… I wonder if i am fine to join the program ?
Thanks
Please refer to this post https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html Our programs are likely to compliment your care but prolapse should be discussed with a medical professional first
Hi Alexa, sorry to hear your surgery failed. Sadly, many surgeries for this problem do fail. I saw one of the top docs for my prolapse and my surgery failed. After a year, I had another doc try to fix the problem with a second surgery. That too failed. Now, I just focus on not lifting, whenever possible, and strengthening my pelvic floor muscles as well as my core.
I like this website! Thank you, Wendy!
I am living with my prolapse until something better comes out that is less invasive and hopefully has better success. Wishing you the best!
Hi Alexa, sorry to hear your surgery failed. Sadly, many surgeries for this problem do fail. I saw one of the top docs for my prolapse and my surgery failed. After a year, I had another doc try to fix the problem with a second surgery. That too failed. Now, I just focus on not lifting, whenever possible, and strengthening my pelvic floor muscles as well as my core.
I like this website! Thank you, Wendy!
I am living with my prolapse until something better comes out that is less invasive and hopefully has better success. Wishing you the best!
Thank you so much for this information. I am excited to start your program before seeing a gyno surgeon for a problem. I have been having problems with sexual pain, urine retention and constipation . My general doc thinks it’s all in my head ( I have not given him permission to do a pap exam) and I have a bad feeling a surgeon will eventually want to cut me open which is just not an option. There is a very sparse number of forward thinking docs in my region. I googled more about prolapse exercises and found your diamond of a site after searching through many “kiegel only” sites. What clued me into the idea that the entire core needed attention was being a follower of a you tube men’s fitness channel and lifting up my left side belly button muscle while urinating to try to completely evacuate my bladder – no kiegel use at all. While the men,s site (Elliot hulse) has a lot of useful theories, it is hardcore lifting and pushing. After trying a few of his workouts and injuring my spine I can really relate with your program’s need to communicate with the muscle before going into heavy training. Thank you for putting this site together!
Have you found anything to help the urine retention that healed it?
Hi Wendy,
I wanted to know if Mutu system would work for me to get a flat stomach.19 months ago I had an emergency hysterectomy after a scheduled because my daughter was breached. Due to back to back surgeries my bowels went into shock and it took awhile for the swelling to go down . I still have a bit of a belly.
Hi Wendy,
I wanted to know if Mutu system would work for me to get a flat stomach.19 months ago I had an emergency hysterectomy after a scheduled because my daughter was breached. Due to back to back surgeries my bowels went into shock and it took awhile for the swelling to go down . I still have a bit of a belly.
Hi Tanera, The Focus program may be safe + may complement your medical care but should only be undertaken with your Doctor’s approval. Given your medical history I can’t make recommendations – you’d need to check with your Doctor + show him / her the program to determine whether it is suitable for you.
Hello
Please how does prolapse heal before pregnancy,will prolapse worsen when one becomes pregnant,I mean someone with prolapse before pregnancy,does it get worse during pregnancy for them
Hey Mama… we’d expressly recommend that you consult with a specialist pelvic health physio for individual attention if you are experiencing any type or grade of prolapse and planning on becoming pregnant again. Whilst prolapse varies in grade and type, the underlying cause (excessive intra-abdominal pressure) is the same, this article explains more about this and steps to help alleviate the symptoms” be sure to take specialist advice to support you during your pregnancy…
Hi Wendy,
I wanted to know if Mutu system would work for me to get a flat stomach.19 months ago I had an emergency hysterectomy after a scheduled because my daughter was breached. Due to back to back surgeries my bowels went into shock and it took awhile for the swelling to go down . I still have a bit of a belly.
Hi Tanera, The Focus program may be safe + may complement your medical care but should only be undertaken with your Doctor’s approval. Given your medical history I can’t make recommendations – you’d need to check with your Doctor + show him / her the program to determine whether it is suitable for you.
Please consult with a doctor or specialist physical therapist as soon as possible Beba, you can find more information + resources here https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Oh Alexa I am so sorry for you. There is a support group on Facebook – search for ‘Pelvic organ prolapse support group’ + tell them I sent you. The MuTu Focus program is recommended by many specialist pelvic physiotherapists to complement or follow medical care, but please only undertake ANY exercise program with a medical specialist’s personal + direct approval.
Hi I’m 24 yrs old and i had a 10.5 lb baby. I think i have some kind of prolapse… i had a vaginal hole but now it looks like meat came down and is covering my vaginal hole.. it’s not coming out i have no pain at all or discomfort how do i know if it’s prolapse? I can hold my pee and everything.
Hi I’m 24 yrs old and i had a 10.5 lb baby. I think i have some kind of prolapse… i had a vaginal hole but now it looks like meat came down and is covering my vaginal hole.. it’s not coming out i have no pain at all or discomfort how do i know if it’s prolapse? I can hold my pee and everything.
Hi Wendy,
sadley the surgery has now failed and am in more pain and discomfort that before. I am awaiting another appointment with my surgeon and hope that they can repair again my uterus is very low, lower than previous. I am just hoping that it hasn’t all failed 🙁
For now I am resting up. Would you suggest swimming to strengthen my pelvis area to aid the support if my organs? I feel so depressed and upset that I will have to undergo more surgery. I rated for three while months and started back swimming and a little low impact exercise. I actually think lifting my children has caused the recurrence 🙁
Anyone else had this happen?
Hi Wendy,
sadley the surgery has now failed and am in more pain and discomfort that before. I am awaiting another appointment with my surgeon and hope that they can repair again my uterus is very low, lower than previous. I am just hoping that it hasn’t all failed 🙁
For now I am resting up. Would you suggest swimming to strengthen my pelvis area to aid the support if my organs? I feel so depressed and upset that I will have to undergo more surgery. I rated for three while months and started back swimming and a little low impact exercise. I actually think lifting my children has caused the recurrence 🙁
Anyone else had this happen?
Have just diagnosed with moderate uterine prolapse and have gone to the womens clinic to locate my pelvic floor muscles as I have obviously been doing my exercises incorrectly for years. for some reason I seem to be very dumb in doing it properly even with help I still come home and tighten my bum muscles and don’t breathe properly has anyone any ideas to help me. I really want to do this
Hi Colleen, the MuTu Focus program addresses first ‘re-connecting’ with your pelvic floor – the vital foundations to being able to restore or strengthen it. What you describe is very common – Focus teaches you how to find the right muscles!
Have just diagnosed with moderate uterine prolapse and have gone to the womens clinic to locate my pelvic floor muscles as I have obviously been doing my exercises incorrectly for years. for some reason I seem to be very dumb in doing it properly even with help I still come home and tighten my bum muscles and don’t breathe properly has anyone any ideas to help me. I really want to do this
Hi Colleen, the MuTu Focus program addresses first ‘re-connecting’ with your pelvic floor – the vital foundations to being able to restore or strengthen it. What you describe is very common – Focus teaches you how to find the right muscles!
Hi can stage 1 and 2 prolapses uterine bowel and mild bladder cause groin pains and muscular skeletal pain? I have been mri and ultra sounded out hip arthrogram negative they can not find anything worms? Gynocologist refuses to say that it can cause these problems! They are not in my head and only happened at the exact same time as the gynocological prolapses advice please
Hi can stage 1 and 2 prolapses uterine bowel and mild bladder cause groin pains and muscular skeletal pain? I have been mri and ultra sounded out hip arthrogram negative they can not find anything worms? Gynocologist refuses to say that it can cause these problems! They are not in my head and only happened at the exact same time as the gynocological prolapses advice please
Please see this page https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Hi can stage 1 and 2 prolapses uterine bowel and mild bladder cause groin pains and muscular skeletal pain? I have been mri and ultra sounded out hip arthrogram negative they can not find anything worms? Gynocologist refuses to say that it can cause these problems! They are not in my head and only happened at the exact same time as the gynocological prolapses advice please
Please see this page https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
Hi Wendy, I am 29 weeks pregnant and already have a 3 yr old. I had no issues with my pelvic floor after having my daughter but since being pregnant again I am suffering urinary incontinence. It’s so embarrassing and I really don’t know what to do and if this will be a long term affect or just during my pregnancy. Please help.
Focus is the completely safe, gentle program for your core + pelvic floor you can use throughout all stages of pregnancy + postpartum. It won’t just get better by itself I’m afraid 🙁
Hi Wendy, I am 29 weeks pregnant and already have a 3 yr old. I had no issues with my pelvic floor after having my daughter but since being pregnant again I am suffering urinary incontinence. It’s so embarrassing and I really don’t know what to do and if this will be a long term affect or just during my pregnancy. Please help.
Focus is the completely safe, gentle program for your core + pelvic floor you can use throughout all stages of pregnancy + postpartum. It won’t just get better by itself I’m afraid 🙁
Yes definitely! Our Focus programme is the right one for you. Take a look under ‘results’ above + watch our testimonial videos – there is a lady there who no longer needs surgery for incontinence!
Yes definitely! Our Focus programme is the right one for you. Take a look under ‘results’ above + watch our testimonial videos – there is a lady there who no longer needs surgery for incontinence!
I have prolapse, but can’t do any more than walk for 15-30 mins a day for exercise because of sevre adrenial fatigue (exercise will cause my condition to worsen at this point.) Do you think just doing kegels with weights or a kegelmaster for the next several months will be enough to prevent the prolapse from getting worst until I can do regular exercises such as squats, etc?
You need to do more than isolate + target the pelvic floor muscles – prolapse is a whole body alignment issue. The Focus program is a great (safe) place to start.
I have prolapse, but can’t do any more than walk for 15-30 mins a day for exercise because of sevre adrenial fatigue (exercise will cause my condition to worsen at this point.) Do you think just doing kegels with weights or a kegelmaster for the next several months will be enough to prevent the prolapse from getting worst until I can do regular exercises such as squats, etc?
You need to do more than isolate + target the pelvic floor muscles – prolapse is a whole body alignment issue. The Focus program is a great (safe) place to start.
Hi, Just been told by GP that I have mild to moderate prolapse – not sure what type. I have two children aged 2 and a half and 4 months. I am feeling quite depressed as I have a lot of conflicting information about surgery. I am going to try physiotherapy at a clinic specializing in women’s health namely pelvic conditions. I am not in pain but am quite upset about the loss of sexual sensation and concerned that things will get worse and lead to possible incontinence, Has anyone had marked improvement from exercise alone?
Hi
I have just had surgery for cystocele, rectocele, enterocele and uterine prolapse all in one. I am 31 years old with 2 children 1 and 3 years. My surgery has gone so well, it’s only been 11 days since the operation and I already see the changes. I had real pain, pressure and back ache all the time and now I don’t feel anything as my body feels normal. The pressure has gone and bowel movements and urine all flows as it should be. I can’t imagine how great I will feel once all healed in 5 weeks or so. I beg anyone with this to have surgery.
My only worry is exercise… I am so active and ran regularly, I also weight trained 3 times a week. I am so worried I will never gain this back? Could you please give me some self help tips to gain strength and advise a time frame in which my previous activities could be achieved again!
I think your post is fantastic!!!!!!!
Hi
I have just had surgery for cystocele, rectocele, enterocele and uterine prolapse all in one. I am 31 years old with 2 children 1 and 3 years. My surgery has gone so well, it’s only been 11 days since the operation and I already see the changes. I had real pain, pressure and back ache all the time and now I don’t feel anything as my body feels normal. The pressure has gone and bowel movements and urine all flows as it should be. I can’t imagine how great I will feel once all healed in 5 weeks or so. I beg anyone with this to have surgery.
My only worry is exercise… I am so active and ran regularly, I also weight trained 3 times a week. I am so worried I will never gain this back? Could you please give me some self help tips to gain strength and advise a time frame in which my previous activities could be achieved again!
I think your post is fantastic!!!!!!!
Thanks Alexa + wow! you have had a LOT to deal with 🙁 I’m so pleased for you that your surgery has been so successful. Now you need to heal + restore, + then strengthen (in that order). I urge you to try our Focus program – it will gently ease your body back to correct alignment + function. Wishing you well + sending you MuTu love + healing x
Hi
I have just had surgery for cystocele, rectocele, enterocele and uterine prolapse all in one. I am 31 years old with 2 children 1 and 3 years. My surgery has gone so well, it’s only been 11 days since the operation and I already see the changes. I had real pain, pressure and back ache all the time and now I don’t feel anything as my body feels normal. The pressure has gone and bowel movements and urine all flows as it should be. I can’t imagine how great I will feel once all healed in 5 weeks or so. I beg anyone with this to have surgery.
My only worry is exercise… I am so active and ran regularly, I also weight trained 3 times a week. I am so worried I will never gain this back? Could you please give me some self help tips to gain strength and advise a time frame in which my previous activities could be achieved again!
I think your post is fantastic!!!!!!!
Thanks Alexa + wow! you have had a LOT to deal with 🙁 I’m so pleased for you that your surgery has been so successful. Now you need to heal + restore, + then strengthen (in that order). I urge you to try our Focus program – it will gently ease your body back to correct alignment + function. Wishing you well + sending you MuTu love + healing x
Hi Wendy,
sadley the surgery has now failed and am in more pain and discomfort that before. I am awaiting another appointment with my surgeon and hope that they can repair again my uterus is very low, lower than previous. I am just hoping that it hasn’t all failed 🙁
For now I am resting up. Would you suggest swimming to strengthen my pelvis area to aid the support if my organs? I feel so depressed and upset that I will have to undergo more surgery. I rated for three while months and started back swimming and a little low impact exercise. I actually think lifting my children has caused the recurrence 🙁
Anyone else had this happen?
Oh Alexa I am so sorry for you. There is a support group on Facebook – search for ‘Pelvic organ prolapse support group’ + tell them I sent you. The MuTu Focus program is recommended by many specialist pelvic physiotherapists to complement or follow medical care, but please only undertake ANY exercise program with a medical specialist’s personal + direct approval.
Hi Alexa, sorry to hear your surgery failed. Sadly, many surgeries for this problem do fail. I saw one of the top docs for my prolapse and my surgery failed. After a year, I had another doc try to fix the problem with a second surgery. That too failed. Now, I just focus on not lifting, whenever possible, and strengthening my pelvic floor muscles as well as my core.
I like this website! Thank you, Wendy!
I am living with my prolapse until something better comes out that is less invasive and hopefully has better success. Wishing you the best!
Great article, great info. I am a Stott Pilates instructor who has done additional training and study in pelvic floor training, as well as a mother of three who has overcome mild stress incontinence through exercise. I agree with most of what you say here except for your take on the “tailbone.” I define the tailbone as the coccyx. I have found it tremendously effective to begin lower body stabilization by “tucking the tailbone”–meaning, to pull the coccyx toward the pubic bone (I sometimes call this “closing the bottom of the abs”) while remaining in neutral spine (so the sacrum/pelvis is not tucked). This article states that the pelvic floor muscles attach to the sacrum, but in fact most of these muscles attach to the inside (anterior surface) of the coccyx. There is a joint between the coccyx and the sacrum, and I have found that closing this joint against some degree of resistance–in conjunction with activating the transverse abdominals and mutifidus–does strengthen the pelvic floor and help alleviate incontinence. It also helps flatten the abs and improve posture. I highly recommend Eric Franklin’s Pelvic Power and blandine Calais-Germine pelvic floor anatomy book for further reading. I also recommend checking out The Women’s Health Foundation’s Total Control Program. It’s great that there are so many people out there bringing focus to pelvic floor issues!
Hi. I was diagnosed with a umbilical hernia, ventral hernia and d.r. When tested for d.r my muscles do close but the ventral hernia pokes through once I sit up or stand up. The doc says the ventral hernia must be addressed so I am getting a repair for that. I do have a splint, I can elevator and hold my muscles pretty well, I can do leg lifts, clams, and all the exercises recommended but still no luck : /
So perhaps fixing the bulge will allow my recti muscles to stay put? This whole pressure concept is new to me. Can a ventral hernia be fixed. I asked the TT lady bbut she didnt answer…just said her program helps with the umblic hernia and d.r though i believe the ventral hernia is keeping my recti muscles from closing??
Have your repair for the hernia if that is what has been recommended by your doctor. And stop doing leg lifts… You’re right – they are all connected. Pressure is the root cause of ALL the issues you have. MuTu Focus is non impact, progressive work that will realign you + reverse the pressure. Surgery + binding won’t work long term if the pressure is still pushing out – you have to fix the cause not just the symptoms – thats what MuTu does! Good luck.
Hi. I was diagnosed with a umbilical hernia, ventral hernia and d.r. When tested for d.r my muscles do close but the ventral hernia pokes through once I sit up or stand up. The doc says the ventral hernia must be addressed so I am getting a repair for that. I do have a splint, I can elevator and hold my muscles pretty well, I can do leg lifts, clams, and all the exercises recommended but still no luck : /
So perhaps fixing the bulge will allow my recti muscles to stay put? This whole pressure concept is new to me. Can a ventral hernia be fixed. I asked the TT lady bbut she didnt answer…just said her program helps with the umblic hernia and d.r though i believe the ventral hernia is keeping my recti muscles from closing??
Have your repair for the hernia if that is what has been recommended by your doctor. And stop doing leg lifts… You’re right – they are all connected. Pressure is the root cause of ALL the issues you have. MuTu Focus is non impact, progressive work that will realign you + reverse the pressure. Surgery + binding won’t work long term if the pressure is still pushing out – you have to fix the cause not just the symptoms – thats what MuTu does! Good luck.
Hi I am 26 weeks pregnant & just came across this – is there any thing I can do at this stage to help avoid all of the above?! Thanks.
Yes you can! Learning now to connect with + engage your core muscles + how to protect your pelvic floor will help a lot! The MuTu Focus program is completely safe for pregnancy – take a look under ‘the store’ above
Hi I am 26 weeks pregnant & just came across this – is there any thing I can do at this stage to help avoid all of the above?! Thanks.
Yes you can! Learning now to connect with + engage your core muscles + how to protect your pelvic floor will help a lot! The MuTu Focus program is completely safe for pregnancy – take a look under ‘the store’ above
Hi I’m 24 yrs old and i had a 10.5 lb baby. I think i have some kind of prolapse… i had a vaginal hole but now it looks like meat came down and is covering my vaginal hole.. it’s not coming out i have no pain at all or discomfort how do i know if it’s prolapse? I can hold my pee and everything.
Please consult with a doctor or specialist physical therapist as soon as possible Beba, you can find more information + resources here https://mutusystem.com/referral-to-a-womens-health-physiotherapist.html
I am suffering a lot of pain in and around my whole lower regions The fullness described above defo rings true too # I have make 3 Drs appointments and chickened out, I’m 29 I have had 2 pregnancies and several illnesses and don’t fancy being poked and prodded for months on end again What is the treatment and also does any body know if its even repairable I will just die if I have to have a finger in my bum and they cant fix it anyway
Go to the doctor Darling. I know its horrible, but ask for a female doctor (its your right to choose) if that makes you more comfortable + explain to her how nervous you feel. Please don’t ignore it or avoid getting checked out due to dreading the appointment. I sympathize – I had terrible hemorrhages after both my births + I totally understand not wanting to be poked about again 🙁 But you must take care of your body + that’s what the doctor are trained to do. Go, have her explain your options + take it from there x
I am suffering a lot of pain in and around my whole lower regions The fullness described above defo rings true too # I have make 3 Drs appointments and chickened out, I’m 29 I have had 2 pregnancies and several illnesses and don’t fancy being poked and prodded for months on end again What is the treatment and also does any body know if its even repairable I will just die if I have to have a finger in my bum and they cant fix it anyway
Go to the doctor Darling. I know its horrible, but ask for a female doctor (its your right to choose) if that makes you more comfortable + explain to her how nervous you feel. Please don’t ignore it or avoid getting checked out due to dreading the appointment. I sympathize – I had terrible hemorrhages after both my births + I totally understand not wanting to be poked about again 🙁 But you must take care of your body + that’s what the doctor are trained to do. Go, have her explain your options + take it from there x
I was diagnosed after my last pregnancy with partial uterine prolapse. Your information is great, especially the exercises (I was just told by my doctor to do lots of kegels!) I know in general my pelvic floor is very weak/off balance – I get terrible SPD pain every pregnancy (so that it becomes painful just to walk around my house!), always have some pain during intercourse, and after months of kegels, still have some leaky bladder issues.
I was also told that doing regular exercise programs (cardio, pilates, even running on the treadmill) were off-limits and would make my condition worse – but I am about 50 lbs overweight and quite eager to shed it! Is it true, am I not allowed to exercise (other than strengthening my core)? And, if this is so, how would I know when I could start real exercise again?
I am now nearing the end of my fourth pregnancy, and I really want to get my body back in shape after this!
Also, wanted to ask you… how soon after birth can your exercise program be started? one week? six weeks? more?
Really appreciate your insights…
Hi Esther, If you body cannot currently hold your insides inside… your bladder leaks + intercourse is painful – you must deal with these issues before you worry about pounding away on a treadmill. Your body is not ready to do ANYTHING that would increase intra abdominal pressure further + that means nothing high impact. But that doesn’t mean you can’t walk! And ‘core exercise’ doesn’t have to mean ‘not proper exercise’! Check out the MuTu Focus program for safe, beneficial core + pelvic floor strengthening through exercises, stretches + alignment adjustments that will put your body back where you want it, + get your body functioning the way its supposed to. Get MuTu focus, get familiar with the concepts + start right away when your baby is born – this about finding muscles + learning how to use your body right – its not ‘working out’. Also, re the weight loss post pregnancy – this is decided by your food choices, not on the treadmill anyway – so follow the ‘clean eating’ rules (look under ‘food + fat loss’ up on the menu above)to get you on the right track. Good luck 🙂 https://mutusystem.com/mutu-focus-program-the-essential-foundations-of-a-flatter-post-baby-tummy.html
I was diagnosed after my last pregnancy with partial uterine prolapse. Your information is great, especially the exercises (I was just told by my doctor to do lots of kegels!) I know in general my pelvic floor is very weak/off balance – I get terrible SPD pain every pregnancy (so that it becomes painful just to walk around my house!), always have some pain during intercourse, and after months of kegels, still have some leaky bladder issues.
I was also told that doing regular exercise programs (cardio, pilates, even running on the treadmill) were off-limits and would make my condition worse – but I am about 50 lbs overweight and quite eager to shed it! Is it true, am I not allowed to exercise (other than strengthening my core)? And, if this is so, how would I know when I could start real exercise again?
I am now nearing the end of my fourth pregnancy, and I really want to get my body back in shape after this!
Also, wanted to ask you… how soon after birth can your exercise program be started? one week? six weeks? more?
Really appreciate your insights…
Hi Esther, If you body cannot currently hold your insides inside… your bladder leaks + intercourse is painful – you must deal with these issues before you worry about pounding away on a treadmill. Your body is not ready to do ANYTHING that would increase intra abdominal pressure further + that means nothing high impact. But that doesn’t mean you can’t walk! And ‘core exercise’ doesn’t have to mean ‘not proper exercise’! Check out the MuTu Focus program for safe, beneficial core + pelvic floor strengthening through exercises, stretches + alignment adjustments that will put your body back where you want it, + get your body functioning the way its supposed to. Get MuTu focus, get familiar with the concepts + start right away when your baby is born – this about finding muscles + learning how to use your body right – its not ‘working out’. Also, re the weight loss post pregnancy – this is decided by your food choices, not on the treadmill anyway – so follow the ‘clean eating’ rules (look under ‘food + fat loss’ up on the menu above)to get you on the right track. Good luck 🙂 https://mutusystem.com/mutu-focus-program-the-essential-foundations-of-a-flatter-post-baby-tummy.html
Thank you so much for this information! It is by far the best I have found.
You’re welcome, I’m so glad it helped 😉
Thank you so much for this information! It is by far the best I have found.
You’re welcome, I’m so glad it helped 😉